What to Expect When You're Expecting Part 1: Debunking Myths about Pregnancy and Tooth Changes
/The host of physiologic changes that occur in women’s bodies during pregnancy leads to a number of changes in the mouth that are good to be aware of. There are also some myths about pregnancy-related tooth changes to address.
Let’s start with the myths:
MYTH 1: Teeth lose calcium to provide for the growing baby’s needs
- There is no mechanism for teeth to lose calcium to provide for systemic needs. If an individual’s blood calcium level is low, the parathyroid glands release parathyroid hormone to increase blood calcium in 3 ways:
1. Mobilization of calcium from BONE by stimulating bone remodeling cells to reabsorb bone minerals and free calcium into the blood.
2. Enhancing absorption of calcium from the small intestine by stimulating production of Vit D in the kidneys. Vit D stimulates synthesis of a calcium-binding protein in the small intestines to increase calcium absorption.
3. Suppression of calcium loss in urine
- Note: As any individual would, expectant mothers will of course want to make sure that they are getting adequate calcium from their diet.
MYTH 2: Pregnancy causes tooth loss / Women lose a tooth per baby
Pregnancy can cause tooth mobility (see below), but the mobility is temporary. If a tooth is lost/needing to be extracted during pregnancy, it would be due to circumstances unrelated to the pregnancy itself (i.e. tooth fracture or infection that would have been present whether the patient was pregnant or not).
Oral changes that CAN be expected during pregnancy:
1. Gingivitis
- Changes in gingival vascularity can lead to an increased sensitivity to plaque and therefore increased swelling/inflammation/bleeding of the gums.
- What should be done: Continue regular gentle and thorough homecare. Keep your regular dentist appointments for cleanings (Dental treatment during pregnancy is safe and recommended! To be addressed in Part 2 of this post). Rinsing with warm salt water may help with the irritation and inflammation.
2. Benign oral lesions
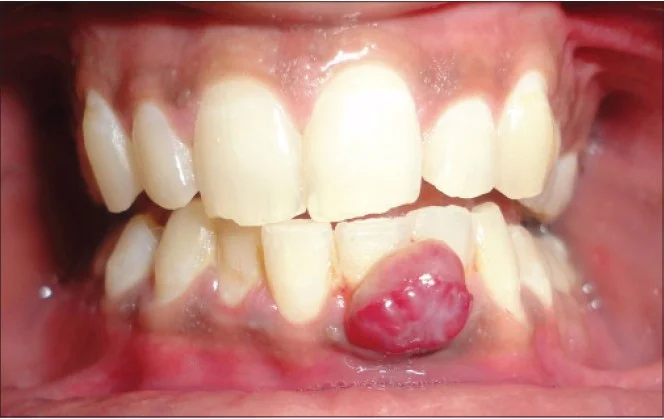
- This type of lesion is known as pyogenic granuloma, granuloma gravidarum, epulis of pregnancy, or pregnancy tumor
- These lesions are thought be be an exuberant tissue response to local irritation (plaque, tartar), or trauma. They occur in about 5% of pregnant women with onset usually in the 2nd or 3rd month. Although they may be referred to as “epulis of pregnancy” or “pregnancy tumors,” they also occur unrelated to pregnancy in men and women. Although they may be alarming in appearance due to being highly vascular, they are benign.
- What should be done: These lesions usually spontaneously regress following pregnancy. If there is severe pain or bleeding or if the lesion interferes with chewing, excision may be needed.
3. Tooth erosion associated with exposure to stomach acid
- As discussed in previous posts, teeth are susceptible to mineral loss (erosion) in the presence of acid. Recognizing that acid reflux and vomiting associated with morning sickness or hyperemesis gravidarum may occur during pregnancy, it is no surprise that erosion of teeth may follow.
- What should be done: Avoid brushing the teeth for 30 minutes after the acid attack in order to avoid scrubbing acid-weakened enamel. Rather, consider neutralizing the acid with a baking soda solution (rinsing with 1 tsp baking soda dissolved in 1 cup of water) to help protect the teeth.
4. Tooth mobility
- Hormone changes that occur during pregnancy lead to temporarily softened ligaments in the body. This includes not only the ligaments in the pelvis to prepare for childbirth, but also ligaments throughout the body, including the ligaments that hold our teeth in the bone. This may lead to temporarily loosened teeth. In the absence of other complicating factors, there should be no tooth loss associated.
- What should be done: Continue to wear retainers or nighttime appliances (night guard, occlusal splint) if you already have one. Otherwise simply know and trust that your teeth will regain their normal stability post-partum.
5. Increased risk of tooth decay associated with diet changes and acid reflux
- Exposure to stomach acid (discussed above under tooth erosion) and typical dietary changes during pregnancy (increased snacking/shorter intervals between eating and increased consumption of carbohydrates or sugary snacks due to cravings) lead to an increased risk for decay.
- What should be done: See post on protective factors here.
6. Periodontitis
- When untreated, gingivitis (discussed above) can progress to periodontitis. Periodontitis is the inflammatory condition of the gums and bone in response to the persistent presence of destructive plaque on the teeth and under the gums. The toxins released by the bacteria and the body’s inflammatory response ultimately results in loss of attachment of gums and bone from the teeth. In advanced cases, teeth may become loose or be lost and bacteremia may result.
- What should be done: Prevent or treat periodontitis by keeping your regular dental appointments during pregnancy. If periodontitis is diagnosed, deep cleanings called scaling and root planing will be recommended. As mentioned, dental treatment during pregnancy is safe and recommended! (To be addressed in Part 2 of this post).
In closing:
Pregnancy brings many anticipated and unanticipated changes. Please be reassured that the oral changes that may occur during pregnancy are temporary, and there are safe ways to keep your teeth healthy in the meantime. Stay tuned for Part 2, which will address safety of dental treatment during pregnancy.